Publications
OPEN examines data, clinical practices and strategies to support better pain management, opioid stewardship, policy, treatment and care.
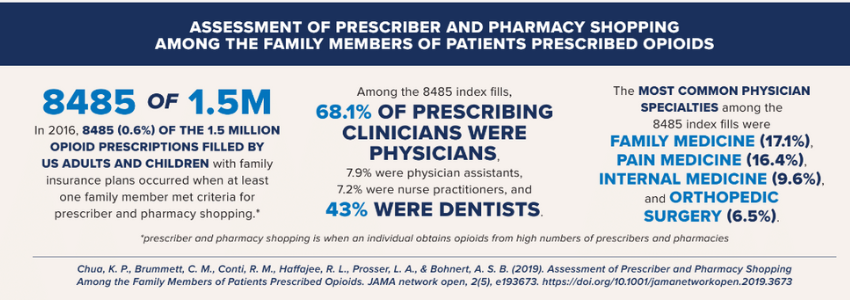
Assessment of Prescriber and Pharmacy Shopping Among the Family Members of Patients Prescribed Opioids
Chua KP, Brummett CM, Conti RM, Haffajee RL, Prosser LA, Bohnert ASB. Assessment of Prescriber and Pharmacy Shopping Among the Family Members of Patients Prescribed Opioids. JAMA Netw Open. 2019 May 3;2(5):e193673. doi: 10.1001/jamanetworkopen.2019.3673. PMID: 31074819; PMCID: PMC6512276.- In 2016, 8485 (0.6%) of the 1.5 million opioid prescriptions filled by US adults and children with family insurance plans occurred when at least 1 family member met criteria for prescriber and pharmacy shopping. *
- Among the 8485 index fills, 68.1% of prescribing clinicians were physicians, 7.9% were physician assistants, 7.2% were nurse practitioners, and 43% were dentists.
- The most common physician specialties among the 8485 index fills were family medicine (17.1%), pain medicine (16.4%), internal medicine (9.6%), and orthopedic surgery (6.5%)
*prescriber and pharmacy shopping is when an individual obtains opioids from high numbers of prescribers and pharmacies
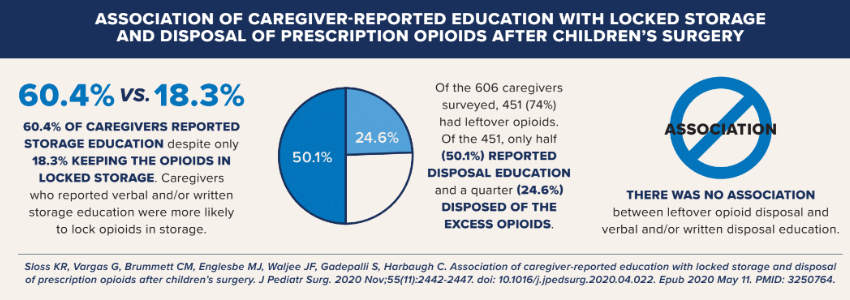
Association of Caregiver-reported education with locked storage and disposal of Prescription opioids after Children’s surgery
Sloss KR, Vargas G, Brummett CM, et al. Association of caregiver-reported education with locked storage and disposal of prescription opioids after children's surgery. Journal of Pediatric Surgery. 2020 Nov;55(11):2442-2447. DOI: 10.1016/j.jpedsurg.2020.04.022. PMID: 32507640.- 60.4% of caregivers reported storage education despite only 18.3% keeping the opioids in locked storage. Caregivers who reported verbal and/or written storage education were more likely to lock opioids in storage
- Of the 606 caregivers surveyed, 451 (74%) had leftover opioids. Of the 451, only half (50.1%) reported disposal education and a quarter (24.6%) disposed of the excess opioids.
- There was no association between leftover opioid disposal and verbal and/or written disposal education.
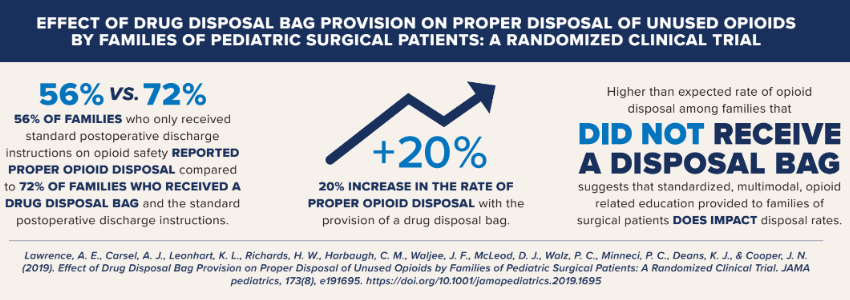
Effect of Drug Disposal Bag Provision on Proper Disposal of Unused Opioids by Families of Pediatric Surgical Patients: A Randomized Clinical Trial
Lawrence AE, Carsel AJ, Leonhart KL, et al. Effect of Drug Disposal Bag Provision on Proper Disposal of Unused Opioids by Families of Pediatric Surgical Patients: A Randomized Clinical Trial. JAMA Pediatrics. 2019 Aug;173(8):e191695. DOI: 10.1001/jamapediatrics.2019.1695. PMID: 31233129; PMCID: PMC6593625- 56% of families who only received standard postoperative discharge instructions on opioid safety reported proper opioid disposal compared to 72% of families who received a drug disposal bag and the standard postoperative discharge instructions.
- 20% increase in the rate of proper opioid disposal with the provision of a drug disposal bag.
- Higher than expected rate of opioid disposal among families that did not receive a disposal bag suggests that standardized, multimodal, opioid related education provided to families of surgical patients does impact disposal rates.
Piloting a statewide emergency department take-home naloxone program: Improving the quality of care for patients at risk of opioid overdose
Dora-Laskey, A., Kellenberg, J., Dahlem, C.H., English, E., Walker, M. G., Brummett, C.M., Kocher, K.E. Published online 28 December, 2021 https://doi.org/10.1111/acem.14435- More than 140 providers were trained in the use of medications for OUD in acute care settings.
- A total of 872 naloxone rescue kits were distributed to ED patients at risk of opioid overdose during the first phase of this project.
- A statewide ED take-home naloxone program was shown to be feasible across a range of different hospitals with varying maturity in preexisting OUD resources and capabilities.
The Opioid Epidemic
Upp, L. A., Waljee, J. F. Published online April 2020. DOI: https://doi.org/10.1016/j.cps.2019.12.005- Opioid-related morbidity and mortality have dramatically increased in the United States over the last several decades.
- Opioid prescribing after surgery has often been in excess, in part owing to the absence of clear prescribing guidelines based on patient-reported pain and opioid-related outcomes.
- Disposal of excess pills after surgery remains low, and unused opioid pills are an important contributor to the opioid epidemic owing to diversion and misuse.
High-Risk Opioid Prescribing Associated with Postoperative New Persistent Opioid Use in Adolescents and Young Adults
Vargas GM; Gunaseelan V; Upp L; Deans KJ; Minneci PC; Gadepalli SK; Englesbe MJ; Waljee JF; Harbaugh CM. High-Risk Opioid Prescribing Associated with Postoperative New Persistent Opioid Use in Adolescents and Young Adults. Annals of Surgery. Published online 27 August 2021. DOI: 10.1097/SLA.0000000000005193- High-risk opioid prescribing practices increased from 34.9% to 43.5% in opioid-naïve patients aged 13-21 from 2008 to 2016; the largest increase was in co-prescribed benzodiazepines (24.1% to 33.4%).
- High-risk opioid prescribing practices, particularly receiving prescriptions from multiple prescribers across specialties, were associated with a significant increase in adolescent and young adult patients’ risk of persistent opioid use.
- Most opioid prescriptions to patients with persistent use beyond the postoperative period were from non-surgical prescribers (79.6%).
New persistent opioid use after surgery in patients with a history of remote opioid use
Agarwal S, Shah A, Gunaseelan V, Sulich C, McAfee J, Urquhart AG, As-Sanie S, Lin J, Waljee JF, Brummett CM. New persistent opioid use after surgery in patients with a history of remote opioid use. Surgery Journal. Published online 8 December 2021. DOI: 10.1016/j.surg.2021.11.008- Among patients not using opioids preoperatively, a history of opioid use was independently associated with new persistent opioid use after surgery, especially those with a history of continuous opioid use.
- Similarly, history of opioid use was independently associated with opioid prescription refill at 1 month after surgery.
- Moderate to high alcohol use was associated with new persistent use as well as opioid prescription refill at 1 month
Association of State Opioid Prescription Duration Limits With Changes in Opioid Prescribing for Medicare Beneficiaries
Cramer JD, Gunaseelan V, Hu HM, Bicket MC, Waljee JF, Brenner MJ. Association of State Opioid Prescription Duration Limits With Changes in Opioid Prescribing for Medicare Beneficiaries. Journal of the American Medical Association Internal Medicine. Published online 9 August 2021. DOI: 10.1001/jamainternmed.2021.4281- Between March 2016 and July 2018, 23 states implemented legislation limiting the duration of initial opioid prescriptions to a maximum of 7 days (17 states limited to 7 days or less, 2 states to 5 days or less, and 4 states to 3 days or less).
- State laws limiting opioid prescriptions to 7 day or less were associated with a reduction in opioid prescribing by 1.7 days per enrollee.
- The state legislation on opioid prescribing primarily targets initial opioid prescriptions provided for acute pain, and we observed decreases that were most pronounced among surgeons and dentists.
Effect of injury location and severity on opioid use after trauma
Baker RC, Brown CS, Montgomery JR, Mouch CA, Kenney BC, Englesbe MJ, Waljee JF, Hemmila MR. Effect of injury location and severity on opioid use after trauma. The Journal of Trauma and Acute Care Surgery. Published online 1 July 2021. DOI: 10.1097/TA.0000000000003138- Among patients admitted for traumatic injury, 8.6% developed new persistent opioid use.
- Patients suffering from extremity and abdominal injuries are at highest risk.
- Maximum individual region injury severity predicts development of new persistent use, whereas total injury severity does not.
Endovascular surgery is not protective against new persistent opioid use development compared to open vascular surgery
Brown CS; Osborne NH; Hu HM; Coleman D; Englesbe MJ; Waljee JF; Brummett CM; Vemuri C. Endovascular surgery is not protective against new persistent opioid use development compared to open vascular surgery. Vascular. Published online 15 June 2021. DOI: 10.1177/17085381211024514- Among opioid-naïve patients undergoing vascular surgery procedures in Medicare between 2009 and 2017, 2.6% of all patients developed new persistent use.
- Undergoing endovascular carotid or venous surgery was associated with an increased risk of NPOU, whereas no differences were found between endovascular and open approaches for peripheral arterial or aortic disease.


