Opioids are strong prescription pain medications with the potential for serious side effects and complications. Common opioid names include oxycodone, hydrocodone, morphine, and codeine. It is important to know that codeine is not recommended for use in children.
Because of their risks, opioids are not usually the starting point to manage acute pain. Over-the-counter medications and non-medication techniques should be the first things used to manage acute pain. Together, they are often enough to manage your child’s pain. If an opioid is prescribed, it is usually only for management of breakthrough pain after surgery.
Breakthrough pain is severe pain despite over-the-counter medications and non-medication techniques. Know that even if you are using an opioid for breakthrough pain, you should still use the over-the-counter medications recommended and nonmedication techniques. This will allow you to use as little of the opioid as possible.
Some opioids already contain acetaminophen. If this is the case, your child may be unable to take over-the-counter acetaminophen with the opioid. Check the label and discuss this with your pharmacist.
Anyone who uses an opioid is at risk for these side effects:
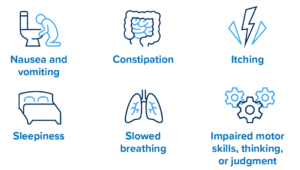
Children who are overweight or have obstructive sleep apnea or snoring have a higher risk of sleepiness or slowed breathing from an opioid. Do not use opioids to help your child sleep.

Common Opioids Include:
| Generic Name | Brand Name |
|---|---|
| Fentanyl | Duragesic* |
| Hydrocodone | Vicodin®*, Norco®* |
| Hydromorphone | Dilaudid® |
| Methadone | Methadose® |
| Morphine | MS Contin®, Kadian |
| Oxycodone | Perococet®*, OxyContin® |
| Oxymorphone | Opana® |
| Tramadol | Ultram®, Ultracet®* |
* Contains acetaminophen (Tylenol). Use caution if you’re also taking acetaminophen separately.
Anyone who uses an opioid, even for a short time, is at risk for dependence, tolerance, misuse, addiction, and overdose. Adolescents are especially at risk for opioid misuse and addiction because the parts of the brain that control impulsiveness and decision-making are still developing. (reference 19) In addition, peer pressure can also affect their behavior. Other factors that increase the risk of opioid use disorder include personal history of depression and/or anxiety and family history of substance use disorder.
When an opioid no longer has the same effect on your child’s pain as it first did, which means they need a higher dose to control pain. For example, if your child is taking an opioid which first worked well for pain, and then later it doesn’t work as well, it does not always mean the pain is worse. Instead, your child may have become tolerant to the opioid.
When your child’s body has started to rely on the opioid to function. This can happen even with using an opioid for a short time period, but the longer your child takes an opioid, the higher the risk. This is one reason why it is important to use an opioid for as short a time as possible. Suddenly stopping an opioid when a person is dependent causes symptoms of withdrawal, such as muscle aches, yawning, runny nose and tearing eyes, sweating, anxiety, difficulty sleeping, nausea/vomiting, and/or diarrhea.
When your child takes the opioid they were prescribed at a higher dose, more often, or for reasons other than which it was prescribed.
When your child develops a brain disease known as Opioid Use Disorder (OUD). People with this condition seek and use opioids even though they are causing them harm.
When your child takes a dose of medication that is too high for them. This affects breathing and can cause your child to stop breathing.
When anyone other than your child gets and uses the prescribed medication. This can happen when you do not safely dispose of an opioid or leave it unattended. Diversion is dangerous because it can lead to misuse, overdose and/or opioid use disorder in others. Sharing or selling an opioid is a felony in the state of Michigan.

Next Page: Non-Medication Options